From COVID testing to prosthetics for zoo animals: 3D printing at USF Health and TGH
USF Health and Tampa General Hospital's innovative use of 3D printing enhances care in several specialties and recently earned national recognition.
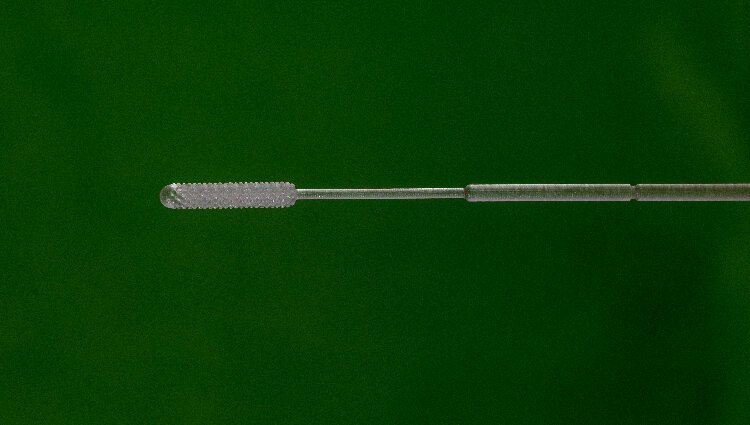
During the height of the COVID-19 pandemic, when nasal swabs couldn’t be found for testing, Dr. Summer Decker and Dr. Jonathan Ford, experts in medical 3-D printing at USF Health and Tampa General Hospital, helped create a swab out of plastic with grooves in the soft tip that proved to hold the virus longer than the typical flocked swabs.
USF Health, Tampa General and their colleagues in the project, Northwell Health in New York and medical 3-D printer maker Formlabs, gave the design criteria and clinical data free to hospitals, clinics and licensed medical device manufacturers around the world, and so far more than 100 million swabs have been produced and distributed in some 60 countries.
In December, the U.S. Patent and Trademark Office honored the USF Health and TGH team’s contributions at the high point of COVID with the Patents for Humanity Award.
As vital as it was in the crisis, the nasal swab is a simple tool compared to the revolutionary three-dimensional creations of the Center for Medical 3D Printing Applications, located in the radiology department of Tampa General Hospital.
Medical 3D printers, which can cost $150,000 to $300,000 or more, can produce exact replicas of a patient’s heart, for example, defects and all. It can show the exact borders of cancerous lesions. Doctors can study the model to plan the surgery. Decker, director of the center and professor in the Department of Radiology at USF Health Morsani College of Medicine, says it can reduce an 11-hour surgery to 3 hours, cutting the time and risk a patient is under anesthesia and lowering the chance of infection.
“They can actually go in and size them and say, I know walking into surgery I’m going to need to use this size, and this is the approach I’m going to be able to do. And have everything planned out.

And that’s how you get from an 11-hour surgery down to three hours because every bit of it has been really planned out,’’ Decker says.
Innovative technology to improve care
Ford, associate professor in the Department of Radiology in the medical school and technical director of medical 3D printing at Tampa General, points out that all the different specialties come through radiology.
“We do a lot of facial trauma reconstruction,” he says. “We can print cutting guides to cut out aspects of it, taking part of someone’s lower leg bone and replace their mandible with it and have it actually fit perfectly. We can do that.”
“For our cardiac stuff, because we can print flexible material, we can then have the heart feel like the heart, the aorta feel like the aorta,’’ Ford says. “We can print that out, hand it to the surgeons and they can practice the procedure, practice with all the devices they’re going to use and make sure they’re going to fit.’’
For complicated pregnancies, they can reconstruct the entire fetus inside the womb so doctors can practice a difficult delivery or an in-utero surgery.
Being able to put the model or “print’’ of a patient’s defective heart in the patient’s hands makes the problem and the procedure clear to them, Decker says. She calls it true informed consent.
“In some of the cases, patients have commented that ‘this is the first time I’ve truly understood what’s going on,’’’ Decker says.
The process
Medical 3D printers create three-dimensional models by printing and building up a series of thin layers of clinical-grade resin in the object’s shape. It’s taken from a computer program that captures images from the patient’s CT and MRI scans and creates three-dimensional images of the area.
It’s a multi-step process, depending on what the model is, Ford says. The more complex the print, the longer it takes. It requires printers in flawless condition and a true expert guiding the process.
“Through some manual, some semi-automated aspects we’re able to tease out the anatomy of interest,’’ Ford says.
He says they meet with the physician and “depending on what they want, what they need, we then will focus on an aspect of the scan, make sure it’s of high enough quality that we can actually do what we need to do. Then, say, if they were doing the mandible, we’d tease out the jawbone and … tease out the tumor that’s on the jawbone.’’
Not all patients have been human. The 3D printing team made a prosthetic for a great Indian hornbill named Crescent at ZooTampa. They made a piece to fit exactly in the hole left by the removal of a tumor at the base of the bird’s casque, a helmet-like extension of its upper bill. They also created a prosthetic beak for a harpy eagle at the Fort Worth Zoo.
Leaders in using 3D printing technology
Having begun the Center for Medical 3D Printing Applications 10 years ago, USF Health and Tampa General Hospital were among the first to start using medical three-dimensional printing applications, traditionally used to train medical students, to prepare doctors for surgery. In 2019, Decker is happy to report, medical 3D printing received its own medical billing code, like other medical devices and procedures.
While it is still not widely used, the field is growing, Decker says, “and we’re really excited that we work nationally with some of the other hospitals on helping it grow as a field.’’
No doubt the swab the team created helped in the effort. Decker says they realized that the materials had all been cleared by the U.S. Food and Drug Administration. The computers and printers they use were all FDA-approved and the material they used was surgical grade, which meant it had already been FDA-approved for it to touch patients.
“So all of the big hurdles had already been addressed,’’ she says.
Todd Goldstein, in charge of the medical 3D printing operation at Northwell Health in New York, helped design the swabs.
“They wanted to help because they were in New York City without any test kits,” Decker says.
The team used Formlabs printers.
“We were able to pull up a clinical trial in two weeks and get data that really changed how the U.S. was able to respond to COVID,’’ Decker says.
Medical 3D printers can already make prosthetic hands, arms and legs. Ford expects that 3D-printed organs that replace failing organs – artificial hearts, for example – will be available in the near future.
“It’s coming,’’ he says. “It’s not there yet whatsoever. But the more complex organs are coming.’’
Ford says that in 2006 medical personnel at Wake Forest University, using a 3D printer, created the shape of a patient’s bladder.
“They seeded it with the patient’s cells and were able to grow a bladder and put it into the patient,” he says. “He’s doing great.’’
The bladder is a rather simple organ, he points out. The heart and those that have a chemical interface, like the pancreas and lungs, are more complex.
“We will get there eventually, but I think they’re probably 10 or 15 years away at least,” Ford says.
For more information, go to USF Health 3D Printing.