The opioid epidemic: Hillsborough County, USF thought leaders look for solutions
"The opioid epidemic is a complex problem and the solution has to be as comprehensive and complex as the problem is," says Dr. Khary Rigg, Assistant Professor in the USF Department of Mental Health and Law Policy. Read more about what he and others are doing to find solutions.
Joseph Cover was prescribed opiates following a car accident in 2002, when he was 21 years old. By the time he turned 22, he was a “pure addict catastrophe” — his words. He spent the remainder of his twenties wondering if he’d live to see his next birthday.
“When it hits you for the first time, you don’t know what you’re dealing with until you’re actually dealing with it. All the sudden I wasn’t working, I wasn’t paying bills, I was racking up debt. I was no longer functioning,” Cover recalls.
We now know that opioid dependence can develop within days of consistent use — but in 2002, many doctors prescribing opiates and patients taking them were not aware of that danger. Hindsight, Cover notes, indicates that he was a “fish in a barrel” for the emergent opioid industry in the United States.
The CDC identifies three waves in the opioid epidemic, beginning in the late 1990s when increased opioid prescription rates precipitated a five-fold increase in overdose deaths between 1999 and 2016. The crisis’ second and third waves — deaths related to heroin and illicitly manufactured synthetic opioids such as fentanyl — followed state and federal crackdowns on prescription pill access starting in 2010.
More than 700,000 people in the U.S. have died from an opioid overdose since 1999. As of 2016, opioid overdoses result in 8.9 deaths every day in the state of Florida. In Hillsborough County, alone, the opioid epidemic continues to put hundreds in the morgue and devastates countless loved ones, year after year.
In spite of what he calls his “delayed adulthood,” Cover earned a marketing degree after he was released from prison in 2010 and launched an environmental nonprofit that now operates worldwide. He’s opioid-free and a registered medical cannabis patient. He’s also married and has a baby on the way. Cover counts himself among the fortunate few: He survived.
Hillsborough County confronts a public health crisis
In 2017, over 500 people participated in the Hillsborough County Opioid Summit, which led to the creation of the Hillsborough Opioid Task Force — a collective of civic leaders, healthcare professionals, law enforcement, and other community stakeholders who devised a strategic plan to combat the public health crisis.
Task Force data indicates a steady annual rise in opioid overdose deaths in Hillsborough, culminating in a 24 percent increase in mortality between 2012 and 2017. Estimates place the death toll at its highest ever in 2018, with over 280 deaths.

“The age group where we’re seeing the most deaths is 17-24. Just seeing the numbers from the medical examiner convinced me that we really need to do something,” says Hillsborough County Commissioner Sandra Murman.
“What’s built into the plan is deliverables, outcomes, and all the metrics involved with it,” she adds.
The Task Force made a bold opening move in August 2018 when Hillsborough County filed a lawsuit against 14 major drug makers and distributors, including OxyContin maker, Purdue Pharma. Mike Moore, the Mississippi-based attorney who is known for leading the litigious strike on Big Tobacco in the 1990s, represents the county.
“Filing the lawsuit was a really important part of the plan,” says Murman. “We hope to get money out of that from drug manufacturers that we can use to increase treatment beds.”
Murman notes that it costs approximately $110 per day to keep an inmate in jail, and adds, “we’re better off spending that money on treatment and services, and having them visit with professionals in medically assisted treatment programs.”
The strategic plan outlined by the Opioid Task Force is overseen by the Behavioral Health subcommittee of the county’s Healthcare Advisory Board. Among its primary goals is to provide opioid users with access to wrap-around treatment services that extend support beyond the “crisis moment” when they find themselves in the emergency room or jail.
“All the pieces are not exactly in place yet, but one of the biggest things we’re working on is creating step-down units at the jail. It’s the first time in our state anything like that’s been done,” says Murman.
HCSO offers support at the jail door to reduce recidivism
The Hillsborough County Sheriff’s Office is in the process of converting a 120-bed work release center that has been out of use since the early 2000s into a 60-120 unit transitional housing facility that will offer substance abuse and mental health services for inmates leaving the jail. Murman expects the step-down facility will open its doors in 2020, following construction build-outs.

“We’re currently working on getting community partners who are willing to help transition that building into a space for anyone who needs support coming out of the jail system or Baker Act facilities in our community. Our goal is to have a treatment unit where we can also wrap-around services that provide education and vocational training, transportation, and safe housing,” says HCSO Jail Division III Major Michael Farrier, who oversees medical and mental health units and substance abuse programming at the jail.
Farrier says that on any given day, the jail has between 50-60 people in its detox units.
“One of the problems you’ll see: we’ll be able to stabilize and detox them, but if there’s not a community providing continuity of care when they’re released, they’ll fall back,” Farrier says.
The HCSO received a $750,000 grant through the Second Chance Act, in partnership with Hillsborough County community partner, ACTS, that enables HCSO and ACTS to launch a three-year program that begins substance abuse treatment in jail and help inmates transition to community treatment centers upon release. The Hillsborough Community Recidivism Reduction Initiative launches on Oct. 1, 2019, with the grant funding for 40 participants.
The Central Florida Behavioral Health Network funded the placement of three case managers from community care facilities (ACTS, DACCO, and the Phoenix House) in the jail to identify participants for other substance abuse programs in the Tampa region.
“Because we can only identify 40 people [for the grant program], I send the rest to those case managers to help place them elsewhere. If the inmate doesn’t meet initial criteria, the case managers can still help them find a program or facility in the community, should they desire to seek treatment. We’ve referred over 280 people since we started in April,” Farrier says.
Two additional case managers have also been assigned to the jail to help enroll participants in the Hillsborough County Health Care Plan.
“We all know addiction is a disease. We understand that people sometimes commit crimes because of their disease — because there are underlying mental health or substance abuse problems that aren’t being addressed — and we understand that as an agency, we have to take a different approach to that these days. We want to do more than take somebody and lock them behind bars and then not do anything to help them,” says Farrier.
Breaking down stigma, silos in the local medical community
Dr. Jayant Rao, an emergency room physician at St. Joseph’s Main, North, and South hospital locations in Tampa, is President of the Hillsborough County Medical Association.

“If someone comes in with a stroke and you’re at a hospital that’s well-equipped to handle these things, you’ll immediately jump on the patient with a crisis team, including radiology, neurology, etc. In the case of substance abuse: An overdose is the moment of crisis. My goal is to have a process to manage these emergent issues — just like how we manage a stroke or heart attack,” says Rao.
The first shift in combating the crisis, Rao says, is to keep patients “opiate naive” as much as possible — in other words, for doctors to prescribe opiate pain killers only when absolutely necessary.
“In the past, we’ve all operated independently in silos. We used to give opioids out for minor pains including toothaches and ankle sprains. … People would come in complaining of severe pain and we wanted to help them, but we weren’t aware of how dangerous it was.”
Now, he says, a prescription drug monitoring program allows doctors to rapidly access patient records to identify whether they have a history with opiates. It’s a step toward breaking down the silos in healthcare.
However, one of the biggest hurdles to combating the opioid epidemic from the front lines remains: most E.R. doctors simply aren’t trained to treat addictions, Rao says. Among the challenges are time constraints in the emergency department and the stigma surrounding substance abuse. Rao understands what many doctors still don’t: Experiences like Cover’s involving multiple relapses are not uncommon. Relapse is often part of the recovery process because the brain isn’t wired for an abstinence-only approach to opiate addiction.
“Relapse can be frustrating for physicians who are trying to help patients. It’s hard to see a person continue to make the same mistakes. At some point, there comes the argument about personal responsibility, where some medical providers are saying, ‘why are we catering to these patients? They don’t want help. It’s a waste of our time and resources.’ But in the ER, we frequently see patients who don’t take the best care of themselves or make the best decisions. We see diabetic patients eating cheeseburgers and drinking milkshakes. We see cardiac and C.O.P.D. patients who continue to smoke. This can be frustrating, but we care for them the best we can,” he says.
In the future, hopefully, addiction will similarly be seen as a chronic disease, Rao says,
Dr. Rao looks toward innovative efforts taking place in emergency rooms across the country — namely, “warm handoff” protocols that help connect patients directly to addiction treatment facilities outside the emergency department. The goal, Rao says, is to offer support that goes beyond delivering a pamphlet and ‘tough-love’ lecture before pushing patients out the door. He aims to prevent another crisis moment that could put the patient back in his E.R. — or the morgue.
Unfortunately, many times the patient isn’t ready to enter addiction treatment directly from the E.R. So in those cases, conversations around harm reduction become very important.
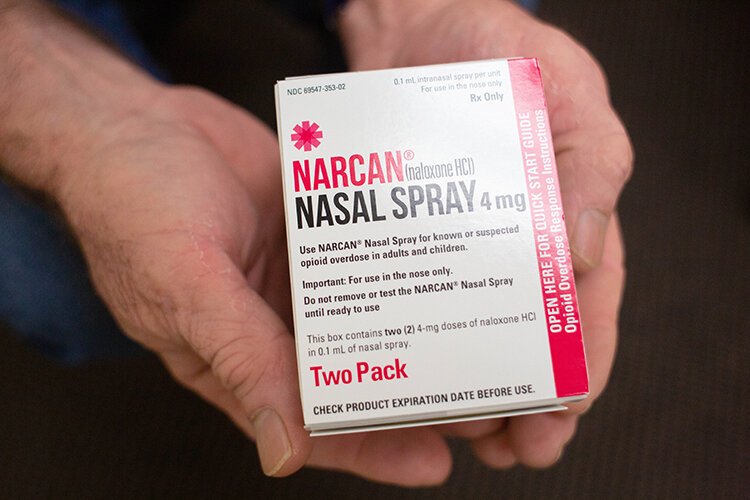
“I’m an idealist and try to help the person in front of me however I can. So, if the patient isn’t ready for definitive treatment, you have to educate them about harm reduction,” Rao says. “You teach them to make sure they have Narcan when they’re using. You teach them to never use alone. You teach them about the dangers of sharing needles. You do what you can to help prevent them from getting HIV or endocarditis from a dirty needle. One hospitalization for endocarditis alone could fund a prenatal program for months.”
Harm reduction saves lives, creates community, and provides pathways for recovery
“The opioid epidemic is a complex problem and the solution has to be as comprehensive and complex as the problem is,” says Dr. Khary Rigg, Assistant Professor in the USF Department of Mental Health and Law Policy, and Faculty Affiliate of the Louis de la Parte Florida Mental Health Institute.

“We spend most of our resources on treatment: downstream approaches with very little attention to prevention and even less to harm reduction. In my opinion, I think it’s to the exclusion of those other more important topics. People who use drugs are people. They’re people who are vulnerable. They need help.”
Dr. Rigg has been conducting substance abuse research for 15 years. He believes that harm reduction — keeping the large percentage of active substance users who are not in treatment safe, by whatever means possible — is the “missing piece” to the opioid epidemic in the United States.
“Historically, the attention has been focused on prevention and treatment. Going back to the War on Drugs in the 1970s through the 1990s, the focus was on prevention. The idea was: ‘Drugs are bad. People who use drugs are bad. People who have a drug problem should be in treatment’,” Rigg says.
“That’s a very dichotomous way of looking at it: There’s prevention and then there’s treatment. But the reality is that there is a big subsection of folks who are using drugs and there are no interventions aimed at them,” he adds.
Matt Zweil, the founder of the Pasco- and Pinellas-based nonprofit, Safe Exchange Tampa, insists that many aspects of the opioid crisis are rooted in a nationwide failure to address mental illness. Opioid addiction, he says, is often a maladaptive coping mechanism caused by underlying mental health issues — not unlike self-harm, or eating disorders like bulimia and anorexia — but bears the most burdensome stigma.
“It’s important to frame the opioid crisis in Florida as a superset of the mental health crisis, but also to recognize that there is very little in the way of resources for people with mental illnesses that are less stigmatized — let alone those with addiction issues,” says Zweil.
“If you are a person who is dealing with depression or an anxiety-related crisis; if you are suicidal — these are things people can understand and empathize with — but they view those struggling with addiction as people apart.”
Zweil founded Safe Exchange Tampa in 2017 in an effort to stanch the spread of HIV, Hepatitis C, and other bloodborne pathogens that are easily transmittable by injection drug use. The organization centers its efforts around the community’s most vulnerable populations, and does so by bringing itself to them.
Safe Exchange Tampa volunteers partner with methadone clinics throughout the region to offer overdose identification and response training. The organization provides free Narcan — the opioid overdose reversal agent currently priced over-the-counter at approximately $250 — to everyone who attends training. Since November 2017, Safe Exchange Tampa has provided approximately 1,000 units of Narcan. As a result, Zweil says the organization has received just over 160 reports of successful overdose reversals to date.
“The reason why we position our work at methadone clinics is because those people are connected to the community of active users. They’re the ones with some of the closest ties to people who are at risk of dying as a result of an overdose,” Zweil says.
“In harm reduction, it’s an unfortunate but necessary evil that we have to do these things not in a proactive, but in a reactive way: We work to provide services that educate and provide guidance to the people who are receptive to it. Our goal is to keep people alive while they are dealing with these maladaptive coping mechanisms,” he adds.
Hillsborough prepares for a syringe exchange program
Zweil lobbied to revise the Infectious Disease Elimination Act (IDEA) to include the entire state of Florida. IDEA, which was passed by the Florida Legislature in 2015, created the state’s first syringe exchange program at the University of Miami — but until July 1, 2019, it remained illegal anywhere else in the state to institute a needle exchange program.
“Syringe exchange is a good policy that doesn’t make sense to people at first,” says Zweil. “The first time I was introduced to the idea, I wholly rejected it. Why would you provide paraphernalia when you need to address the root cause of the issue?”
Zweil adds, “but the first argument is strictly financial. The cost of treating HIV and Hepatitis C is borne by taxpayers, and approximately 20 percent of HIV cases in Florida are transmitted from drug users sharing dirty needles. From a more humanistic perspective, the fact is that syringe exchange is able to offer people a service and a material they can’t get anywhere else. It’s there to help them regain a foothold in mainstream society. It’s a chance they wouldn’t otherwise have to eventually return to being a constructive member of society.”
On June 23, Florida Governor Ron DeSantis signed Senate Bill 366 into law, allowing for county commissions to authorize sterile needle and syringe exchange programs statewide.
Commissioner Murman admits that she, too, was skeptical about needle exchange initially — but says the numbers coming out of Miami are compelling. Since instituting the IDEA Exchange program in 2016, Miami reports 1,075 overdose reversals and more than a quarter-million syringes collected. It’s also the only place in Florida seeing a decrease in opioid-related mortality while death tolls spike across the state.
“I was skeptical in the beginning because I don’t want it to look like we’re promoting drug abuse — but we’re not. We’re trying to actually decrease it,” Murman says.
“If we can get people to come to the door to exchange needles — I don’t want to say we want to ‘capture’ them in the sense that we’ll hold them against their will — but at least we’ll be able to find out who these people are out there who are OD’ing. We’ll have a chance to reach them before they get to the morgue.”
Having witnessed quick results in Miami, and with the recent passing of the IDEA expansion, Murman says Hillsborough County is already in the process of implementing its own syringe services program.
“Our Healthcare Services staff is working to put something together that we can take to our Behavioral Health Task Force and County Commissioners that lays out exactly what a program will look like,” says Murman.
Because state law prohibits the use of county or state funds for syringe services programs, Murman explains, “we’re reaching out, now, to see if anybody is interested in being a host site for the needle exchange program. Whoever hosts it will be funding it — or getting grant funding. This will absolutely be a very collaborative effort.”
USF data heads take on opioid deaths with innovative tech
“I’m a researcher,” notes USF’s Dr. Rigg, “so I’m not dogmatic about any one intervention. I’m about ‘what does the evidence say?’ Let’s do that. Let’s do what the evidence says.”
At USF, Dr. Rigg says researchers in the Department of Mental Health Law and Policy are using CDC grant funding and working with ACTS to explore technology-based solutions that might help prevent opioid overdoses and aid medicine-based treatment efforts.
Today’s protagonists in the fight against the opioid epidemic can agree, thanks to overwhelming data, that an abstinence-based approach to the drug is ineffective. From the emergency room to the jailhouse, professionals on the front lines of the epidemic now encourage medication-based treatment using buprenorphine and naloxone (the active ingredients of the prescription drug, Suboxone), which work together to prevent withdrawal symptoms associated with opiate addiction.??”The data shows folks do well on Suboxone. Some studies show it cuts overdose in half or folks on it. But one of the major problems with medical treatment is that folks tend to discontinue treatment if they’re managing it on their own. It’s a maintenance medication that you have to dose every other day. Patients tend to waver or discontinue treatment early,” Rigg says.
Dr. Rigg is a co-investigator on MySafeRX, a program in partnership with Harvard University that he anticipates will launch this fall at USF, following IRB (Institutional Review Board) approval. MySafeRX is an app Suboxone users can install on their phone that helps monitor their use and utilizes motivational intervening to help patients stay on their treatment schedule. When users check-in with the app, they are able to access a lock box that stores their medication.
“It’s trying to help resolve barriers that might prevent people from taking their medication. We’re testing that intervention to see if it improves engagement and retention on buprenorphine because once we can have people stay on longer, it can translate to fewer deaths,” Rigg says.
Dr. Rigg is also working on a project at USF that uses a wearable biosensor device — similar to a FitBit, he says — to improve treatment outcomes with opioid users in an outpatient setting. The biosensors will measure factors including skin temperature, heart rate, and breath rate, and will help researchers understand what the patient experiences, and how feasible biosensors could be in detecting opioid relapse.
The three-year project is slated to launch near the end of 2019.
For more information, click on the links below:
- Center for Disease Control
- Henry J. Kaiser Family Foundation
- Hillsborough County Commissioner Sandra Murman
- HSCO Major Michael Farrier
- Second Chance Act Grant Program
- ACTS Florida
- Central Florida Behavioral Health Network
- Hillsborough County Health Care Plan
- Dr. Khary Rigg, USF
- Louis De La Parte Florida Mental Health Institute
- Safe Exchange Tampa
- IDEA Exchange
- MySafeRX