Top research taking place in Tampa leads to national recognition for innovation, patents
It may not have the reputation of Silicon Valley or Princeton, but the Tampa area, led by the University of South Florida, is becoming a national center of technical and scientific innovation, largely but not solely in the health care field.
What if a surgeon could see through a patient’s skin and look at the internal organs while operating?
What if a person using a wheelchair could open up a tray table to hold a notepad, or maybe a beer at a ball game, and push a button to retrieve the computer from his backpack?
What if a bridge builder could scan a freshly poured concrete foundation pillar and tell whether it’s setting properly, while the mix of cement, aggregate and water can still be fixed if there are flaws?
What if an oncologist could tell whether chemotherapy will save a lung cancer patient before having to put the patient through the grueling, destructive drug regimen?
Those are all things that could be happening soon – or in some cases already are happening — because of work done in the Tampa area by innovating engineers, physicians and scientists.
It may not have the reputation of Silicon Valley or Princeton, but the Tampa area, led by the University of South Florida, is becoming a national center of technical and scientific innovation, largely but not solely in the health care field.
In June, USF placed 10th nationally and 13th worldwide on the National Academy of Inventors’ annual list of the top 100 universities for patents granted during 2014. The university received 104 patents, putting it into the same league with MIT, Stanford, Johns Hopkins and the California university system.
The National Academy of Inventors itself was founded by Paul Sandberg, USF’s Senior VP for Research, Innovation and Economic Development.
Sanberg, a neurologist who holds 111 patents, is best known for research on repairing brain damage caused by stroke or other brain diseases, including using stem cells from bone marrow and umbilical cord blood. Sanberg has a Ph.D. in Biological Science from Australian National University
Sophisticated research takes place every day
Besides USF, the inventions are coming from places like the H.L. Moffitt Cancer Center & Research Institute in Tampa and even the Lions Eye Institute in Ybor City.
Some are based on the most sophisticated research in science and engineering.
But others are devices that seem so simple and obvious, once they’ve been suggested, that even their own inventors are astonished they don’t already exist.
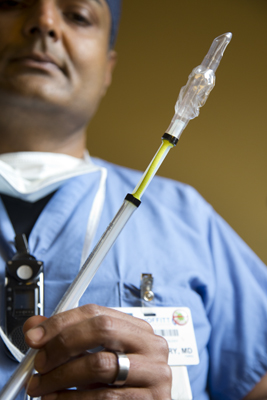
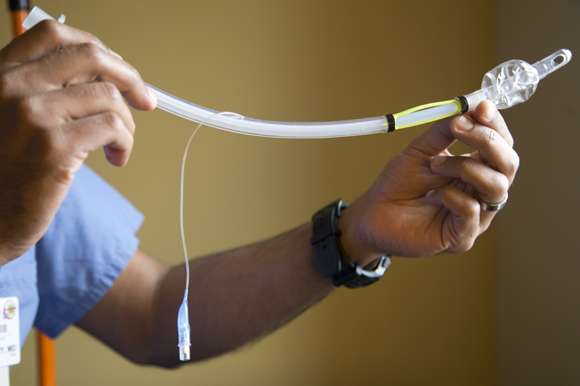
“When I show it to people, the reaction is, ‘How come I didn’t think of it?’ ” says Moffitt Anesthesiologist Tariq Chaudhry of his invention, a new kind of endotracheal tube, or breathing tube.
While Moffitt researchers routinely delve into bewilderingly sophisticated molecular biology, genetics and chemistry, Chaudhry’s invention is a simple, cheap piece of plastic tubing.
But it can prevent a sudden, unpredictable complication during surgery that can turn a routine procedure into a stay in intensive care, and provoke malpractice lawsuits.
His new kind of breathing tube invention allows a surgeon to test whether a patient can breathe on his own before removing it. That matters because a breathing tube, often required during surgery, can irritate the airways of an unconscious patient, causing them to swell shut as soon as it’s removed. The patient is then unable to breathe; the surgeon then must reinsert the tube and send the patient to the ICU, at a cost of perhaps $10,000 a day.
It’s also a potential lawsuit.
“The problem can’t always be predicted, but if your son or daughter goes in for a same-day procedure and they end up in the ICU, it’s hard for the physician to justify what’s happened,” he said.
“I’ve been in the OR for 14 years now and this is one of the things where I’ve seen my colleagues struggle and patients suffer,” or die, in some cases, says Chaudhry, a graduate of Liaquat Medical College in Pakistan who completed a fellowship at the University of Massachusetts in Cardiac Anesthesia and served as a resident at Pakistan Institute of Medical Sciences and Tufts University of School of Medicine.
The tube could be on the market within a few months, and Chaudhry expects it will add $3 or $4 to the $10 cost of a standard endotracheal tube.
Another simple invention that came out of USF is a folding tray table for a wheelchair, invented by Mechanical Engineering Professor Stephen Sundarrao, one of the founders of a USF center on technologies to assist the disabled.
He’s also seeking to market a motor-driven device to retrieve a backpack hanging on the back of the chair, so the user can store and use objects without having to ask someone for help.
Sundarrao says commercialization of such products can be harder than inventing them, partly because of the restrictions on medical equipment that insurance and government health programs will cover.
A local former accounting professor, Stuart Pinnock, is seeking to market the two wheelchair accessories through a startup, Life Enabling Tecnhologies.
“I couldn’t believe these things didn’t already exist,” says Pinnock, who has an MPA from the University of Texas at Austin and a B.S. and Ph.D. in Accounting from Florida International University. “How long have we had tray tables on airplane seats?”
Making major advances in helping people see
The Lions Eye Institute, meanwhile, recently served as the facilitator for what could be a major advance in treatment of eye diseases.
Thanks to work done this summer at the institute, located in Ybor City, it may soon be possible for scientists for the first time to preserve the retina of a human eye donated after death, for research and testing on currently incurable diseases that cause blindness.
It could even be the first step in transplanting a retina, the part of the eye that actually “sees” by reacting to light, although such an achievement is far in the future, says Mitch McCartney, scientific director at the institute.
A human retina becomes non-viable, or dies, within four hours after death, says McCartney, who graduated from the University of Guelph in Ontario, earned an MS at the University of Western Ontario and did post-doctoral research at the University of Tennessee, Memphis and the University of Louisville at the Kentucky Lions Eye Research Institute.
McCartney is working with Daniel Lindgren, president of Nevada-based OcuScience, who has developed an instrument that bathes a removed retina in a solution saturated with oxygen and nutrients, while he used light to stimulate the cells and measure their response – an “electroretinogram.” Lindgren gets responses similar to those from living eyes.
Lindgren came to Tampa for his work because the local eye institute specializes in collecting, dissecting and freezing donated eye tissue, including other parts of the eye for transplant.
There was also another reason – unlike most universities, the institute, a charitable organization, didn’t demand a cut of the eventual proceeds from Lindgren’s work.
But that work means it can now be possible to test medications on living retinal tissue.
Some inventions require cross-disciplinary thinking
An invention by USF’s Richard Gitlin comes from what he considers a particularly productive kind of research, the overlap between two different academic disciplines – in this case, electronics and surgery.
Working across disciplines, he says, researchers can provide their colleagues with fresh, outside perspectives and recognize new applications for their knowledge.
Gitlin had a distinguished career in telecommunications, largely with Bell Labs, where he was co-inventor of the digital subscriber line.
Then about 15 years ago, he had robotic kidney surgery performed by the then-new da Vinci machine. He was impressed, and began discussing it with surgeons.
One problem in laparoscopic surgery – surgery performed with electronically controlled instruments inserted through a small opening in the body, often in the navel – is simply having space inside the body for devices the surgeon uses, including cameras, lights, power and communications cables and cutting tools.
Gitlin, an expert on sending information over distances, worked with a team including surgeons and other electronics experts to create a “distributed robotic network” that, in effect, dismantled the da Vinci machine into separate components communicating wirelessly.
The result is the MARVEL system, or “Miniature Anchored Robotic Videoscope for Expedited Laparoscopy.” It allows a surgeon to work with several tiny robotically controlled cameras with integrated light sources, cutting implements and control arms, while electronic controlling equipment and video displays are conveniently spaced around the operating theater.
Its multiple cameras can produce broad, internal views from inside the patient, instead of the narrow, restricted views laparoscopic surgeons normally get. That helps prevent errors such as nicking a nearby artery, and allows the surgeon to work more quickly, a major consideration in any kind of surgery.
The internal views can even be projected onto the patient’s body, producing, in effect, an X-ray vision view. However, Gitlin says the main use of that feature so far is for training.
A start-up company to market the device is currently raising capital, and Gitlin, who has a BS in Electrical Engineering from City College of New York and an MS and a Ph.D. from Columbia University, hopes for clinical trials in 2-3 years.
But anyone who drives on the new connector between Interstate 4 and the Selmon Expressway is already benefitting from another invention coming out of USF – a “thermal integrity profiler” used to discover whether a concrete foundation pillar or bridge piling is setting correctly.
Any construction worker is likely to know that concrete produces heat as it sets.
But USF Civil Engineering Professors Gray Mullins and Stanley Kranc realized that by measuring the uniformity of that heat, they could determine whether the concrete was setting correctly, without “inclusions” – flaws that would weaken the pillar. Mullins earned bachelor’s, master’s and doctoral degrees in Civil Engineering at USF. Kranc earned a Ph.D. in Mechanical Engineering and Astronautical Sciences and a B.S. in Science Engineering at Northwestern University in Illinois.
Their device consists of sensors distributed in a tube extending the length of the pillar, which detect heat variations that indicate non-uniform setting of the cement — before it hardens and while it can still be detected.
The technology has already been used on highway bridges in Milwaukee, Cleveland, Indianapolis and Darlington, S.C., as well as in Tampa’s Crosstown Connector.
Determining if treatments will work — before they are given
By comparison to Gitlin’s cross-disciplinary work and Sundarrao’s bright ideas, a new class of anti-cancer chemicals developed at Moffitt was the result of the kind of painstaking, step-by-step research more common in pure science.
Biochemists Ernst Schonbrunn, a Moffitt researcher who completed a master’s degree at the University of Bochum in Germany and a Ph.D. as well as post-doctoral training at Max-Planck Research Unit for Structural Molecular Biology in Hamburg, and Nicholas Lawrence (Ph.D. in Organic Chemistry, Cambridge University) started with a target — BRD4, for bromodomain-containing protein 4, a group of proteins known to be important in the origin of cancers.
Using what was known about the protein, they tested one compound after another to find those that inhibited its effect on cells. The result: a class of chemicals that appear to attack several kinds of solid and blood cancers. They hope to see clinical trials within three years.
As oncologists know all too well, some of the treatments they use are so damaging to patients they can, in some cases, kill the patient before they kill the cancer.
That’s particularly frustrating, says Moffitt Molecular Biologist Douglas Cress, because with certain types of lung cancer, very few patients actually benefit from the standard chemotherapy.
“But physicians will still give it to them because there’s a small number that do benefit,” he says.
Working on that problem, Cress developed a diagnostic test based on the patient’s genetic signature to determine whether the chemotherapy is likely to help.
Because it’s a diagnostic test rather than a drug, it doesn’t require FDA clinical trials, but does require a different kind of FDA approval. Moffitt hopes to begin using the test in 2016 on its own patients.
After that happens, “We hope word gets out,” says Cress, who has a B.S. from Virginia Polytechnic Institute and State University and a Ph.D. from Michigan State University and completed post-doctoral work as a fellow at Duke University Medical Center. “Oncologists have said they want a test like this.”
By comparison to USF, which reaps scores of patents a year, Moffitt is just getting started in the field of patenting research, says Haskell Adler of Moffitt’s Office of Technology Management and Commercialization.
“We’re a young office,” he says.
Moffitt holds 58 patents and has applied for 366.