NIH trial offers COVID vaccines to high-risk allergy patients
The University of South Florida in Tampa is recruiting patients with and without allergies to receive the COVID-19 vaccine as part of a clinical study.
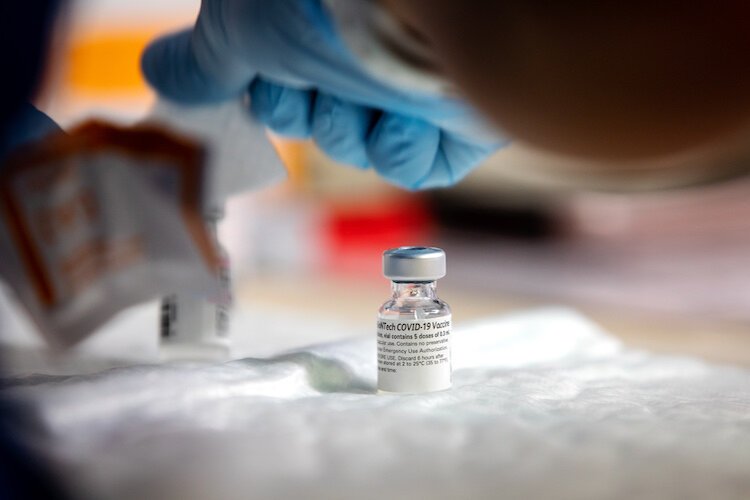
People with life-threatening allergies may be able to take the COVID-19 vaccine at the University of South Florida as part of a government-funded study.
USF’s Asthma, Allergy and Immunology, Clinical Research Unit, has been looking to recruit some 120 allergy sufferers and healthy individuals to participate in the National Institutes of Health’s clinical double blind randomized placebo controlled trial. It already has administered the Moderna, Pfizer, or a placebo to around 30.
“It’s been a real struggle to get people enrolled,” says Dr. Thomas Casale, principal investigator for the study that began in May. “I think by the time the study started the majority of the patients that wanted to be vaccinated were vaccinated. The rest of them have vaccine hesitancy for whatever reasons.”
The trial is to include those with systemic allergies who have a history of anaphylaxis, an acute allergic reaction, according to Michelle Twitmyer, clinical research coordinator at the USF clinic.
Patients may be allergic to foods or insect stings, points out Dr. Casale, a USF Professor of Medicine and Pediatrics, who also serves as chief medical advisor to the McLean,VA-based Food Allergy Research and Education organization.
The control group includes people without significant allergies, who could be considered healthy.
The vaccines are the same as those administered at pharmacies, but trial participants take a blood test before and after and must remain at the clinic for an hour and half for observation, Twitmyer says.
A physician knowledegable about treating severe allergic reactions is at the clinic at 13801 Bruce B. Downs Blvd., Suite 505, located a short distance from AdventHealth Tampa.
“It’s different than if you would pull up to the pharmacy and pull up your sleeve,” he says. “There’s much more scrutiny and oversight of the patients after they get the injection.”
According to the Centers for Disease Control, anaphylaxis is reported rarely following COVID vaccinations. Guidelines call for an observation period of 30 minutes for people with a history of “immediate allergic reaction.”
Study participants who receive the placebo on their first visit are given either the Moderna or Pfizer vaccine on their second visit. They are asked to return for a third visit to complete the vaccination process.
“What happens is basically we have a pharmacy that allocates the vaccine.
Neither we nor the patient know what the patients get,” Dr. Casale explains.
The goal of the study is to see if the allergy sufferers are at a greater risk for developing an allergic reaction to the vaccine, Dr. Casale says.
To be eligible, participants must be between 12 and 69 years of age. While they cannot be pregnant or have COVID-19 at the time, the study accepts those who have recovered from COVID.
The trial excludes those who could suffer adverse reactions because of medication or who have a medical condition like severe uncontrolled asthma.
“It’s a pretty wide open study,” he says.
There have been no severe reactions in the trial thus far. The study is expected to remain open until they get enough participants, Dr. Casale adds.
Those interested in participating should contact the clinic at (813) 631-4024.
















