What to expect when you’re expecting in the time of COVID-19
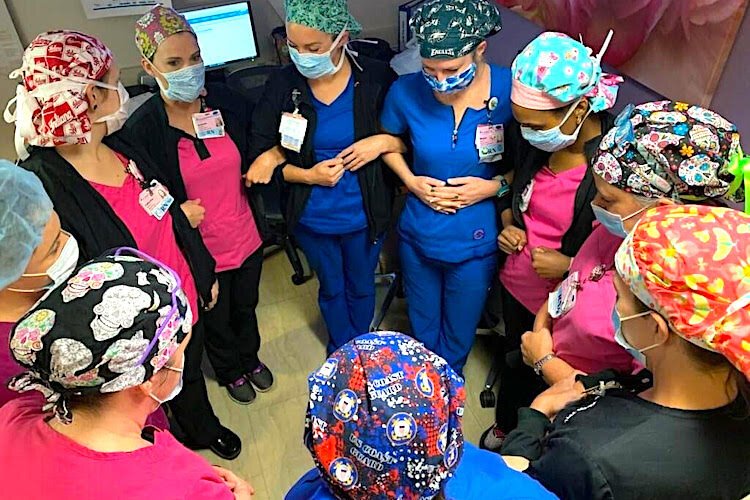
Retired OB/GYN Dr. Bruce Shephard interviews Becky Allen, a certified labor and delivery RN, about her experiences dealing with pregnant patients in labor and delivery at St. Joseph’s Women’s Hospital in Tampa under CDC guidelines surrounding COVID-19.
Fourth in a series.
The National Institutes of Health (NIH) is studying COVID-19’s effect on pregnancy outcomes in the U.S. The study will assess the risk of pregnant COVID-19 patients transmitting the virus to their babies and monitor the newborns until they are discharged from the hospital. The following interview by retired OB/GYN Dr. Bruce Shephard of Becky Allen, a certified labor and delivery RN, provides a nursing perspective for what pregnant patients can expect in labor and delivery at St. Joseph’s Women’s Hospital in Tampa under current CDC guidelines.
Dr. Shephard: You are one of the most experienced nurses at St. Joseph’s Women’s Hospital, one of the largest women’s hospitals in the southeastern U.S. How did you first become interested in the nursing field?
Nurse Allen: When I was 18, our neighbor, who was the nurse educator on the med-surg (medical-surgical) unit at what was then Humana Women’s Hospital talked to me about the nursing profession and was mentoring me in that direction. Just after I graduated high school, she helped me get my first job as a secretary in the med-surg unit, and then I transferred to the newborn nursery. And during this time, I was taking credits for the nursing program and graduated in 1994. After that, my interests led me to the mother-baby unit, the postpartum floor where moms and their newborns room together. I worked there for six years.
Dr. Shephard: So, your education gave you the total childbirth perspective beginning with the care of the newborn and then in dealing with moms who had just delivered at a time when moms and their babies were still separated most of the time. When did you first start working on Labor and Delivery?
Nurse Allen: It was in 2000 and I’ve been here ever since. I really loved working in the postpartum Mom-Baby unit and the teaching, but I felt I needed more of a challenge. I love the whole birth process and really do enjoy helping women bring life into the world. It never gets old, so I enjoy coming to work every day. This definitely became my calling.
Dr. Shephard: And with all this experience, you also have a designated role as a mentor for nurses just starting to work in Labor and Delivery. What’s that like?
Nurse Allen: Yes, I have been a Preceptor in Labor and Delivery for 18 years and we work with each of our interns for six months. They follow you during this time and you teach them everything you know. So yes, I’ve mentored a lot of Labor and Delivery nurses and some of my interns have moved on to become midwives.
Dr. Shephard: And now with COVID, how has this pandemic changed nursing in Labor and Delivery?
Nurse Allen: All of nursing has been impacted. When we arrive in the morning our temperature is taken as soon as we walk in the door. We then do a three-minute scrub. It is recommended we change into fresh scrubs as soon as we come in, change out of our scrubs when we leave our shift, and once at home, remove all clothing before coming into the house and immediately shower.
Dr. Shephard: How are you screening labor patients for COVID?
Nurse Allen: We are testing every patient for COVID-19 before every delivery using a nasal swab. Given the nature and immediacy of what we do, we use rapid testing to process the specimen in-house, which provides results within hours. If needed, we may also do a second test, the slightly deeper nasopharyngeal swab that has a higher sensitivity but takes longer to process.
Dr. Shephard: And for COVID positive patients, what personal protective equipment (PPE) are you using in their deliveries?
Nurse Allen: If we know the patient has tested negative, we use the usual mask and gown. For patients testing positive, we have a completely different process and use N95 masks along with face shields.
Dr. Shephard: Now in the COVID era, what visitor policy changes have been made in Labor and Delivery?
Nurse Allen: We have put in safeguards to help protect the health of patients, team members, physicians and the community. Currently, Labor and Delivery patients regardless of their COVID-19 status are allowed one visitor, which is typically the husband or significant other. If a patient wishes to use a doula, the doula would be their one visitor allowed in the delivery room. All visitors have their temperatures taken and are screened for symptoms of COVID-19. Once a patient is admitted, her visitor is asked not to leave the hospital during their hospital stay.
Dr. Shephard: This must have a tremendous impact on families.
Nurse Allen: It does. For example, if a sick newborn is transferred to the NICU, currently only one person is allowed to visit, which means only one of the parents can see their baby in the NICU. We recognize that there are multiple important members of a patient’s support team who are missing from hospitals at this time, and we look forward to identifying ways to welcome them back into our hospitals safely.
Dr. Shephard: NPR recently reported that medical workers are seeing more anxiety and depression among pregnant patients. Are you seeing that as well?
Nurse Allen: Definitely seeing anxiety, especially whenever we test them for COVID. They ask a lot about the results and they’re very, very relieved once they know they’re COVID negative. Some patients are anxious about not having more than one visitor with them during their delivery.
Dr. Shephard: And anxiety for nurses, too. I’m thinking about the many patients who arrive in active labor. You just don’t have time to get test results if they come in in active labor and deliver quickly.
Nurse Allen: Yes, as you know there’s a lot that has to be done prior to delivery and we may not have time to get test results back for patients who come in already in active labor.
Dr. Shephard: That must have been quite worrisome. Is the hospital testing health care personnel?
Nurse Allen: Yes, if we’ve come in contact with a COVID positive patient and are symptomatic.
Dr. Shephard: The American College of Obstetricians and Gynecologists (ACOG) has advised that COVID-19 does not appear to pass from mom to baby during pregnancy, labor or delivery, and is not in itself a reason to have a cesarian birth. However, there was a Canadian report of an infant born by cesarian who tested positive for COVID, one of a very few reported cases of transfer from mom to baby. At present, at St. Joseph’s Women’s Hospital, what is the care for newborns of COVID positive patients?
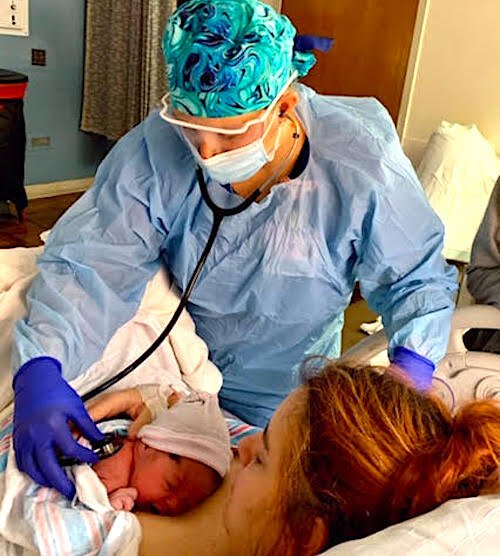
Nurse Allen: The process for caring for newborns delivered by COVID positive patients, whether for a vaginal birth or a cesarian, is the same. Our NICU team is present during the delivery and will transport the newborn to the NICU for evaluation and continued monitoring.
Dr. Shephard: So how is breastfeeding managed in a patient who has COVID, knowing that, at present we really don’t know if women who are sick can pass the virus through breast milk.
Nurse Allen: It’s pretty much a shared decision between the patient, her family and the health care team. In every case, we encourage moms who are COVID positive to wear a surgical mask to minimize risks to her baby.
Dr. Shephard: You and I have worked together going back to the HIV/AIDS era. Does this remind you of some of the stress often felt among health workers in treating those patients during that time?
Nurse Allen: Absolutely. Especially before we started testing every patient for COVID. There was a fear of the unknown. We were treating every single patient as if they could be positive and we were then using full PPE for everyone. It would get very hot when you’re pushing with a patient for two hours and you’re sweating through your clothes.
Dr. Shephard: The Journal of the AMA Psychiatry and other media have reported widely on increased psychological stress experienced by nurses and other health workers since the pandemic’s outbreak. Is that the case at a facility like St. Joseph’s Women’s Hospital, which tends to have a younger, healthier patient population?
Nurse Allen: You know, even in obstetrics, it’s been a little bit nerve-wracking and has caused some anxiety. I do have to say that BayCare (Health System) has done a very good job of making sure that we are very protected. In the beginning we heard about this national mask shortage and we were concerned about that. We wondered, are we not going to get enough masks? But that has not been the issue at all. BayCare has done a great deal — a lot of new processes, a lot of meetings — to get it right with their policies and procedures. This is an unknown territory so they have been developing new policies as we go, following the CDC Guidelines, and doing their best to see that we are protected.
Dr. Shephard: From my own experience delivering babies, I know that precise nursing procedures are critical to safety and quality. Every second counts.
Nurse Allen: Yes. We have a specific process created just for transferring COVID positive patients from triage to labor and delivery or to the operating room. Everybody goes through drills to make sure that we’re comfortable for whenever we do come in contact with these patients. We know exactly what to do. For COVID positive patients, the process is for one nurse to stay in the room with the laboring patient the entire time while a second nurse outside of the room, the “runner,” brings supplies or medications. In Labor and Delivery, there are dedicated “negative pressure” rooms for COVID positive patients that are specially ventilated to reduce the aerosol spread of the virus.
Dr. Shephard: With all that’s going on in a busy Labor and Delivery unit, how is it possible to maintain social distancing with so many nurses and health care personnel working in that space?
Nurse Allen: It’s challenging to always be six feet apart, but we are doing our very best to maintain distancing to minimize the risk. And, when we are in close quarters, such as during our morning and afternoon huddles or at the nurse’s station, where computers are in close proximity, we are always wearing a mask. In the operating room or with deliveries, there’s no way realistically to stay six feet apart.
Dr. Shephard: As a frontline worker, how has your job impacted your own family life?
Nurse Allen: My family, especially my parents and in-laws are older, and I have not been around them at all except to see them from a distance from one end of the driveway to the next. The first time I was close to my mom was Mother’s Day and we actually hugged. That was after two months. And we both cried. With my husband and daughters living at home with me, I have to change my clothes in the garage and shower before they are even allowed to give me a hug or say hello to me. I was really anxious when I was exposed to a COVID positive patient, concerned about exposing my family to the virus. Employee health had me monitor my temperature regularly, and to notify them immediately if any signs or symptoms developed.
Dr. Shephard: Any final thoughts you would like to share with pregnant patients who are out there knowing they may come into the hospital in labor tonight?
Nurse Allen: Just know we are doing our best in taking all precautions to make sure they are protected and we are protected during their stay, and that we will be doing everything we can do to make sure their delivery process goes smoothly during the time that they are with us in the hospital. We are there for you.
Dr. Shephard: Thank you so much, Becky, for sharing your nursing experience and knowledge about a very special time in so many families’ lives, and one with more challenges than ever.
Becky Allen is an RN who has worked as a Certified Labor and Delivery nurse at St. Joseph’s Women’s Hospital for 20 years. Bruce Shephard is a retired Tampa Obstetrician-Gynecologist and Affiliate Associate Professor, Department of Obstetrics and Gynecology, USF, Morsani College of Medicine.
83 Degrees Media’s series on local physicians working in the time of COVID-19:
- First: Dr. Jose Montero, infectious disease specialist
- Second: Dr. Jay Rao, ER physician
- Third: Dr. Sylvia Campbell, surgeon
- Fourth: Becky Allen, Registered Nurse